Correspondence Worsening myopathy associated with ezetimibe in a patient with McArdle disease
Transcription
Correspondence Worsening myopathy associated with ezetimibe in a patient with McArdle disease
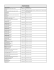
Q J Med 2005; 98:461–464 Correspondence Worsening myopathy associated with ezetimibe in a patient with McArdle disease and aspirin was started. His lipid profile slightly improved (Table 1) but remained above recommended levels according to his estimated cardiovascular risk score. Given the absence of muscular symptoms and the low level of creatine kinase (CK), we added ezetimibe 10 mg/day to his therapy. For the first three months it was well tolerated. CK levels slightly increased, with no weakness or muscular cramps. The patient remained stable for 20 weeks, when he started to complain of fatigue, with impairment of exercise tolerance. Four weeks later, CK levels dramatically increased, and the patient eventually reported slight myoglobinuria and severe weakness. No drugs other than those scheduled had been taken, and he had carefully avoided physical exertion during this period. Ezetimibe was discontinued, and the patient recovered uneventfully. CK levels returned to previous values after 4 weeks, and the patient remains stable 6 months later. Table 1 Clinical and biochemical profile at baseline and development Total cholesterol HDL cholesterol LDL cholesterol Triglycerides CK Creatinine Clinical symptoms Baseline 8 weeks 12 weeks 16 weeks 20 weeks 24 weeks (ezetimibe stopped) 28 weeks 287 34 199 271 837 0.80 No 232 35 160 183 3261 0.90 No 224 39 150 176 1047 0.90 No 240 38 162 201 4360 1.00 No 245 38 172 177 3100 1.00 Mild weakness 237 38 163 181 21370 0.90 Severe weakness Myoglobinuria 316 36 NA 337 1123 0.90 Fatigue Normal values: total cholesterol 110–200 mg/dl; triglycerides 45–200 mg/dl; HDL-c 40–80 mg/dl; LDL-c 60–155 mg/dl; CK 25–190 U/l; creatinine 0.5–1.30 mg/dl. NA, not applicable. The Author 2005. Published by Oxford University Press on behalf of the Association of Physicians. All rights reserved. For Permissions, please email: journals.permissions@oupjournals.org ! Downloaded from by guest on November 24, 2014 Sir, McArdle disease (MD) is the most common disorder of muscle carbohydrate metabolism, caused by mutations in the gene that encodes myophosphorylase.1 Only striated muscles are involved, hence the clinical picture of exercise intolerance, muscle cramps and myoglobinuria secondary to rhabdomyolysis. This predisposition to rhabdomyolysis may exclude the use of certain drugs in MD patients. Ezetimibe, an inhibitor of intestinal cholesterol absorption, is well tolerated, and no adverse muscular effects have been reported to date.2 An overweight 45-year-old White man, diagnosed with MD by biochemical profile and muscular biopsy, with essential hypertension, type 2 diabetes mellitus, hypercholesterolemia and hypertryglyceridemia suffered a non-Q-wave myocardial infarction. Treatment with low fat and low calorie diet, insulin, ramipril, bisoprolol 462 Correspondence Myotoxicity is a well known side-effect of statins, with a reported incidence of 1–7%.3 No cases of rhabdomyolysis due to monotherapy with ezetimibe have been described. However, myopathy triggered by ezetimibe in patients taking statins has been documented in two patients.4 Although MD is a known cause of rhabdomyolysis, the present case strongly suggests that myotoxicity may be elicited by ezetimibe, and poses the question of whether ezetimibe may trigger muscular damage by mechanisms that are presently unknown. J. Perez-Calvo Servicio de Medicina Interna Hospital Clinico Universitario ‘‘Lozana Blesa’’ Zaragoza Spain F. Civeira-Murillo Hospital Universitario ‘Miguel Servet’ Zaragoza Spain References 1. Lebo RV, Gorin F, Fletterick RJ, Kao FT, Cheung MC, Bruce BD, et al. High-resolution chromosome sorting and DNA spot-blot analysis assign McArdle’s syndrome in chromosome 11. Science 1984; 225:57–9. 2. Bays HE, Moore PB, Drehobl MA, Rosenblatt S, Coth PD, Dujovne CA, et al. Effectiveness and tolerability of ezetimibe in patients with primary hypercholesterolemia: pooled analysis of two phase studies. Clin Ther 2001; 23:1209–30. 3. Evans M, Rees A. The myotoxicity of statins. Curr Opin Lipidol 2002; 13:415–20. 4. Fux R, Mo¨rike K, Gundel UF, Hartmann R, Gleiter CH. Ezetimibe and statin associated myopathy. Ann Intern Med 2004; 40:671–2. doi:10.1093/qjmed/hci074 Discordant public and professional perceptions on transparency in healthcare Sir, Transparency is becoming a major issue in healthcare.1,2 Recent work shows substantial differences between views of physicians and those of the public Figure 1. Effect of a disclosure policy upon hospital image, as perceived by the public and by physicians. Downloaded from by guest on November 24, 2014 Ana Cabello Departamento de Anatomı´a Patolo´gica Hospital Universitario ‘12 de Octubre’ Madrid Spain e-mail: mibh-jperez@hcu-lblesa.es on medical errors:3 while the public views open reporting as a very effective way of reducing errors, physicians prefer confidentiality. We conducted a survey to evaluate the potential contribution of a disclosure policy to hospital image. Our findings shed additional light on the discordance of opinions between physicians and the public. We conducted a phone survey (in Hebrew, Russian and Arabic) of a representative sample of the Israeli public (n ¼ 570) using random-dial software. Respondents were asked to predict the effects of a transparency policy upon public image of hospitals and doctors, and also to what extent physicians report mistakes. In addition, we conducted 115 face-to-face interviews of physicians with questions similar to those of the public survey, in three major teaching hospitals (two from Israel, one from the US). They included 53 residents, 54 attending physicians (from internal medicine, surgery and gynecology), six department heads and two hospital directors. The majority of the public indicated that an open disclosure policy would enhance the image of hospitals (Figure 1). By contrast, a majority of physicians predicted that disclosing mistakes would damage the image of the hospital (p50.001 vs. the public). American and Israeli physicians had similar distribution of opinions. Since Israel has a markedly heterogeneous population, we examined whether ethnic or social groups might have different answers. In all subgroups, including Russians, Arabs, and people with low or high levels of education, the majority consistently responded that transparency would benefit hospital image. Both the public and physicians thought that disclosure to patients of individual mistakes by